Facilities & Treatment
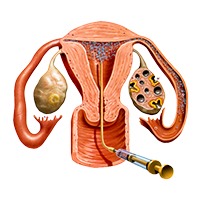
Ovulation Induction
Ovulation induction refers to the use of medication to regulate ovulation by increasing the number of eggs released from the ovaries and thereby boost the chance of pregnancy through either timely sexual intercourse or artificial insemination.
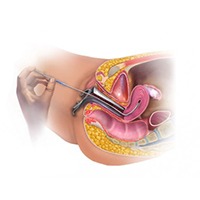
Intra Uterine Insemination (IUI)
Intrauterine insemination (IUI) is a simple fertility treatment where the ‘washed’ and concentrated sperm is placed directly in a woman’s uterus, putting it closer to the egg, increasing chances of pregnancy.
Embryo Freezing
Embryo freezing refers to the process of storing embryos in liquid nitrogen at a low temperature of -196 degree Celsius to be used later in the same patient from whom the embryo was retrieved.
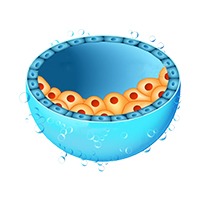
Blastocyst culture and transfer
Blastocyst culture refers to growing the embryos in the laboratory for two more days after which the blastocyst embryos are transferred to the woman’s uterus on
Day 5
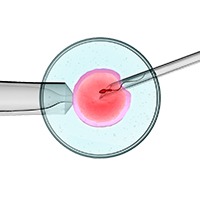
Intracytoplasmic Sperm Injection: ICSI
Intra cytoplasmic sperm injection (ICSI), a procedure similar to IVF, involves direct injection of sperm into the eggs obtained from IVF. A single sperm is injected by an embryologist directly to each egg in this procedure in a laboratory.
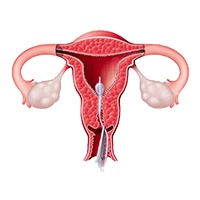
HSG (Hysterosalpingography)
Hysterosalpingography (HSG), also known as uterosalpingography, is a radiologic procedure where the radiologist looks at a woman’s uterus and fallopian tubes to check the shape and patency
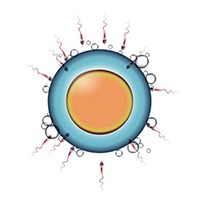
IVF
In Vitro Fertilization (IVF), the most popular type of assisted reproductive technology (ART), where eggs collected from a woman’s ovaries are fertilized in laboratory conditions and transferred to the uterus.

Oocyte cryopreservation
Oocyte cryopreservation, is a method used to preserve reproductive potential in women wherein the woman's eggs (oocytes) are harvested from the ovaries, frozen unfertilized and stored for later use.
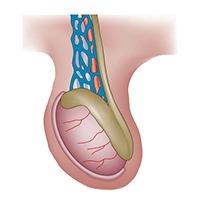
PESA, TESA, TESE, MESA and micro-TESE
Sperm retrieval is recommended for men who have little or no sperm in the semen, or men who aren't able to ejaculate any sperm due to damaged tubes in their testicles or any other genetic problem.

Sperm Freezing
Sperm freezing is the procedure whereby sperm cells are frozen to preserve them for future use. Stored sperms can be frozen indefinitely until needed for assisted reproductive procedures.
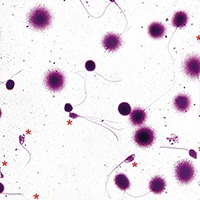
Sperm DNA fragmentation Test
The test provides a reliable analysis of sperm DNA integrity that may help to identify men who are at risk of failing to initiate a healthy pregnancy.
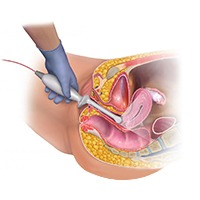
Trans Vaginal Sonography
A transvaginal sonography or ultrasound, also called an endovaginal ultrasound, is a safe procedure used by doctors to examine internal organs in the female pelvic region.

High-risk Pregnancy Care
A woman has a high-risk pregnancy when she or her baby or both of them are at an increased risk of developing health problems during or before delivery, or if the mother has an existing condition that could affect childbirth.
3D Ultrasound Scans for Fertility Testing and Treatment
Ultrasound scans play a major role in pregnancy, right from the stage of confirmation to the final trimester. For fertility testing and infertility treatment, latest technology
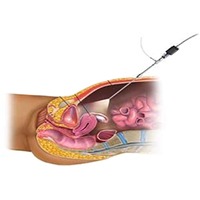
Diagnostic and advanced operative hysterolaparoscopy
An essential tool for the evaluation of female infertility. This tool gives a detailed and direct visualization and analysis of the uterine cavity, endometrium, tubal morphology and uterine and ovarian pathology.
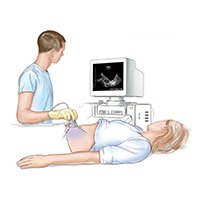
Trans Abdominal Sonography
Trans abdominal sonography is a procedure used to examine the organs through the abdominal wall where an ultrasound transducer is pressed firmly against the skin of the abdomen by trained specialists in internal medicine, radiologists or sonographer.

MICRO TESE
Micro-Dissection TESE (MicroTESE) is an invasive procedure utilized to locate sperm in men with Non-Obstructive Azoospermia or severe testicular failure.

PGT
Pre-Implantation Genetic Testing is a sophisticated scientific method of screening single cells from embryos to identify genetic defects and chromosomal disorders within embryos created using In Vitro Fertilization (IVF) such that they are not transferred to the child.

ELECTRONIC WITNESSING SYSTEM
Electronic Witnessing system is an advanced technology that prevents mismatch of samples in an IVF process, thereby ensuring the happiness of embracing your biological child.
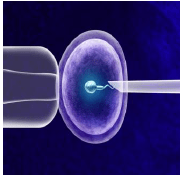
LASER ASSISTED HATCHING
Laser Assisted Hatching is a scientific method used in In Vitro Fertilization to improve the chances of implantation of the embryos onto the uterine lining.

